 Last month the New England Journal of Medicine published an article (link) about the effects of steroid injections in the spine and in particular, repeated prescription of such procedures. It confirms questions in my mind.
Last month the New England Journal of Medicine published an article (link) about the effects of steroid injections in the spine and in particular, repeated prescription of such procedures. It confirms questions in my mind.
Working with clinics around the country and overseas, we act as a hub for patients with chronic back issues to call and find their nearest IDD Therapy provider (non-invasive spinal decompression and mobilisation originating in the late 1990s to address the failings of traditional traction to treat targeted spinal segments).
Naturally, we only hear from patients for whom other treatments have not worked. That does not mean of course that all those treatments are universally ineffective, in the same way that if someone does not achieve a “succesful” outcome with IDD Therapy, it does not mean that nobody else did.
However, the issue we hear repeated by patients is the manner in which injections are so often provided in isolation of structured rehab.
To receive an injection a patient must have a chronic condition and must go through many stages to actually get one – from GP to physio, back to GP, referral to consultant, MRI referral, back to consultant, referral for injection … and all this over many months, if not years before an injection is given.
It seems like madness to me and a recipe for long term chronic back pain.
Improving Cost-Effectiveness of Injections
I am not debating the merits of injections which are generally administered to treat inflammation, but serious questions arise about the cost-effectiveness of steroid injections when given in the absence of structured rehab to address the cause of the inflammation.
The true cost of a spinal injection is not just the cost on the day, but every consultation and every bit of paper to manage that process through the patient journey. Each injection must surely cost several £thousand in real terms.
Some patients will have an injection and be completely pain free, others will see no change and either return to their doctor or not return (which some incorrectly read to mean the patient must be better) and some will be worse.
In a situation where a patient does return for more treatment, surely a better process should be provided rather than to repeat something which at best has only been shown to offer temporary benefit and at worst either no change or worse.
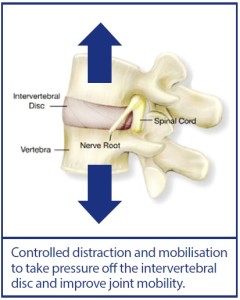 When manual therapy (MT) and exercise alone (allowing for variances in quality of MT) are insufficient to elicit a response for a patient with a disc-related condition, it will be far more cost-effective to prescribe patients with a course of 10 or 20 sessions of IDD Therapy with MT and exercise via NHS physio, rather than to send people into “pain management” programmes with injections.
When manual therapy (MT) and exercise alone (allowing for variances in quality of MT) are insufficient to elicit a response for a patient with a disc-related condition, it will be far more cost-effective to prescribe patients with a course of 10 or 20 sessions of IDD Therapy with MT and exercise via NHS physio, rather than to send people into “pain management” programmes with injections.
A number of years ago I attended a meeting of the Society of Back Pain Research, I can’t remember if it was the one in Helsinki or at Keele University. A number of studies were presented showing that there were no long term benefits of steroid injections for back pain and leg pain.
A senior committee member of the Society was then asked whether in the context of an evidence-based driven service and in light of the studies being presented, was it possible to justify the use of such injections?
The answer burned an imprint in my memory as it was coming from a respected pillar of the spine community:
“I have a clinical intuition that they are effective and … patients ask for them”.
Returning to the calls we receive every day. Patients are desperate. We hear people talking about turning to faith healers, witch doctors, they try everything. Everyone hears about injections so before people try the “alternative” treatments, we might reasonably ask is it any wonder people “ask for an injection”.
I know surgeons and patients. The merits of injections are not questioned, but it does seem to me that in light of issues raised in articles like the one in the NEJM, it makes far more sense to provide a comprehensive course of targeted treatment and rehab with IDD Therapy, before (or in conjunction with) injections to achieve better outcomes for patients. And it will cost decidedly less in the long run.
http://www.nejm.org/doi/full/10.1056/NEJMp1511754
Note – Medical Research seeks to isolate the effectiveness of individual treatment modalities. Therefore if two treatments are given simultaneously, scientists are uncomfortable because it is difficult to pinpoint which element was effective.
Scientists will test combinations of treatment together, but usually the focus of the treatment is one clear variable e.g a cancer cell. The problem when it comes to back pain is that there are so many elements that it can be nigh on impossible to isolate individual variables and the extent to which each contributes to dysfunction and pain.
I am not advocating a scatter gun approach to treatment, rather the combination of treatment tools which have specific goals. So if injections are given with an aim to treat inflammation, it can only improve the chances of successful outcomes if at the same time, the disc is decompressed and segmental mobility improved with IDD Therapy. And from that point, exercise, manual therapy and all the other aspects of a treatment plan can be included for improved long term outcomes and cost-efficiency.
http://www.nejm.org/doi/full/10.1056/NEJMp1511754
See more about how IDD Therapy differs from traditional traction – click here




